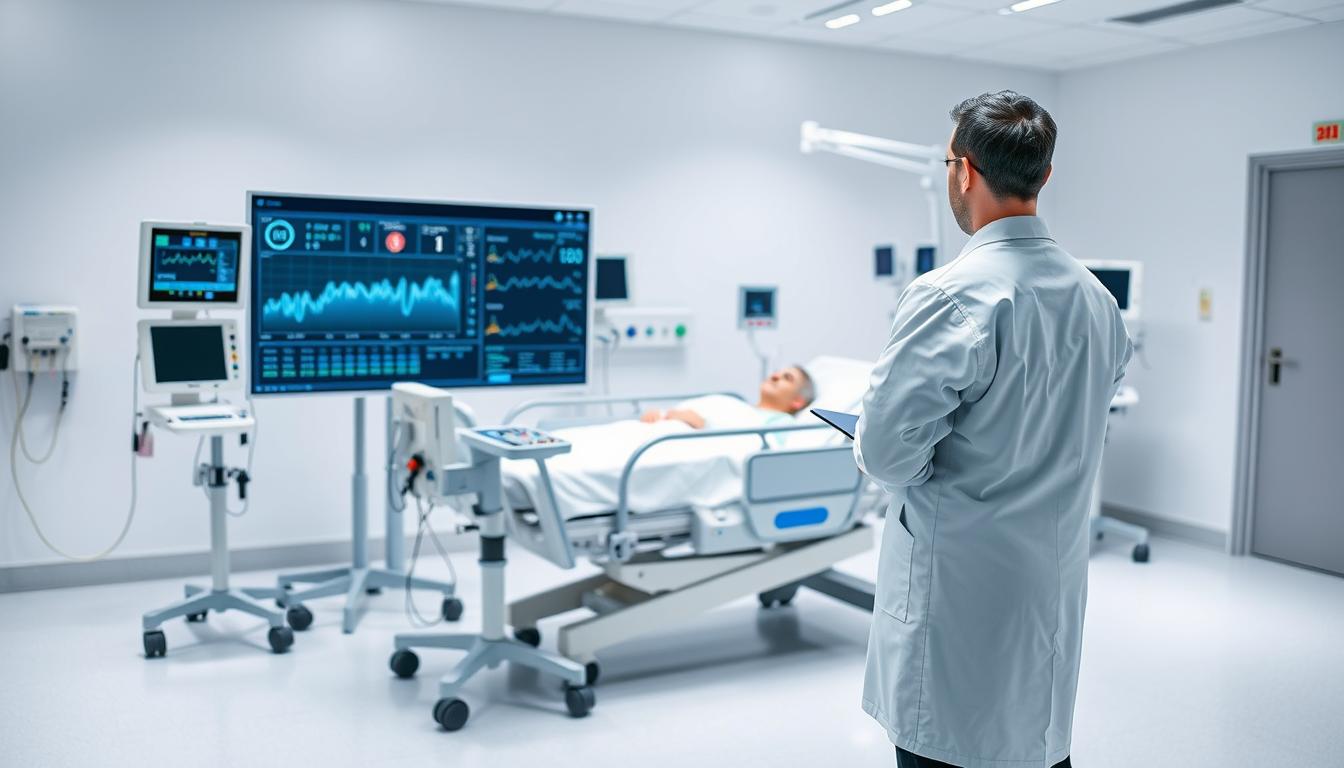
When a college coach noticed a starter stalling in the last quarter, he did more than bench the player. He checked real-time metrics and saw subtle shifts in load and recovery. That small flag led to a rest day and, weeks later, fewer missed contests for the team.
This is how modern performance care starts — with timely data that turns concern into action.
The category has moved from simple step counters to integrated IoT systems that synthesize sensor streams into clear guidance for teams and individuals. Brands like Catapult, STATSports, WHOOP, Oura, and Polar show how continuous monitoring can support injury prevention and better player availability.
Iottive stands out as an end-to-end partner for BLE-connected platforms, cloud analytics, and mobile apps that help translate raw metrics into safer training cycles and measurable returns.

Key Takeaways
- Modern devices blend sensors, cloud, and analytics to reduce risk and boost performance.
- Nearly half of pro injuries are preventable with real-time data and timely decisions.
- Buyers should seek validated solutions that show measurable reductions in missed play.
- Iottive offers BLE app development and scalable IoT platforms for sports teams.
- Secure handling of health data builds trust and long-term adoption across the industry.
Why AI-Powered Sports Watches Matter Right Now
Real-time data from continuous monitoring changes how staff protect players. Nearly 50% of professional injuries are preventable when teams spot load and stress early. That fact turns population-level stats into individual actions.
From monitoring to action: steady streams of heart rate, load, and recovery scores let coaches make low-latency decisions. When fatigue builds, staff can cut minutes, delay high-intensity drills, or mandate recovery days. These small changes reduce soft-tissue injuries and keep performance stable across a season.

Teams justify investment with fewer lost training days and more consistent availability. Practical buy-side checks matter: comfort, battery life, reliable sensors, and easy syncing for staff tablets and phones.
How this works in practice
- Consistent monitoring transforms the “50% preventable” stat into earlier, personalized interventions.
- Real-time transmission enables prompt tapering when fatigue spikes, lowering risk and healthcare costs.
- Iottive’s BLE and mobile-cloud integration supports low-latency flows so coaches act on clear, timely signals.
| Metric | Action Trigger | Team Benefit |
|---|---|---|
| Heart rate variability | Drop vs. baseline | Enforce recovery; fewer soft-tissue injuries |
| Load accumulation | Threshold exceeded | Reduce minutes; preserve long-term performance |
| Sleep score | Consistent low scores | Reschedule high-intensity training |
Understanding the Tech: IoT, AI, and Wearable Sensors in Sports
A compact array of sensors now captures movement, sleep, and muscle activity to inform daily training choices.
Core sensor stack: GPS maps movement, HRV tracks autonomic balance, IMUs (accelerometer + gyroscope) log biomechanics, and EMG measures muscle activation. Each stream feeds risk profiling and readiness scoring.

Bluetooth Low Energy handles continuous streaming from wrist units to phones, while ANT+ and Wi‑Fi sync bulk files. Edge models send instant alerts on the band; cloud analytics run cohort analysis and long-term trend models.
How signals become insight
- Preprocessing and calibration align timestamps and sampling rates to avoid false alarms.
- CNNs extract spatial features; RNN/LSTM models parse time-series to spot gait changes and fatigue.
- Firmware, mobile apps, and secure APIs must interoperate so coaching staff trust the analysis.
- Choose devices by sport: GPS-heavy for field play, IMU-rich solutions for court work, EMG for rehab.
Pipeline summary: acquisition → preprocessing → feature extraction → classification → alerts and dashboard metrics that guide performance and recovery decisions.
AI sports watch, IoT wearable injury prediction, athlete smart device
To move from guesswork to guided action, platforms now aggregate data from multiple body locations and validated sensors.
What counts as an athlete smart device: team-grade solutions deliver higher sampling rates, rugged housings, and exportable raw files. These systems prioritize accuracy, calibration tools, and documented APIs over consumer convenience.

An advanced watch often doubles as an edge hub, collecting streams from chest straps, foot pods, and smart textiles. That fusion boosts analytics quality and lets staff run fatigue and recovery models with confidence.
Common applications include risk scoring, recovery tracking, session RPE validation, and technique cues from IMU signatures. Open SDKs and clear export options matter for integrating team workflows and third‑party analytics.
| Team-grade | Consumer-grade | Coaching impact |
|---|---|---|
| High sampling, validated sensors | Lower sample rate, closed files | Actionable metrics and fewer false alerts |
| Calibration tools, rugged fit | Comfort focus, limited tuning | Reliable long-term monitoring |
| APIs, multilingual apps | Proprietary apps only | Scales across rosters and languages |
Privacy and consent frameworks let staff trend health while protecting rights. Modular platforms let organizations start with individuals and scale to full teams without replatforming. Iottive integrates custom BLE apps and cloud services so buyers tailor applications by roster, sport, and workflow.
How AI Predicts Injuries and Prevents Overtraining
Modern pipelines translate continuous heart rate and motion streams into timely risk signals. Raw data is ingested from sensors, then cleaned and synchronized to remove noise. Features such as HRV trends, stride symmetry, and load accumulation are extracted for modeling.
From HRV and gait to deep learning: models often use LSTM or convolutional architectures to spot temporal patterns. Edge inference can trigger instant alerts while cloud models refine risk over days and weeks.
From HRV and gait to deep learning: the injury prediction pipeline
Pipeline steps are simple to describe and critical to get right:
- Raw sensor ingestion and timestamp alignment.
- Preprocessing and feature extraction (HRV, ACWR, gait metrics).
- Model inference (e.g., LSTM for time series) and confidence scoring.
- Coaching alerts with suggested actions and contextual data.

Explainable models and transferability across sports
Review of 68 studies shows meaningful predictive power: soccer RCT AUC=0.87, team sport DNNs AUC~0.85, and cohort accuracies >80% with IMUs and HRV. Those results support practical use when models are validated and transparent.
| Threshold | Signal | Recommended action |
|---|---|---|
| HRV drop >20% | Autonomic stress | Reduce intensity; schedule recovery day |
| ACWR >1.5 | Rapid load increase | Taper minutes; modify drills |
| Gait asymmetry >10% | Biomechanical instability | Neuromuscular rehab; technique work |
Common pitfalls include false positives, sensor placement drift, and limited cross-sport generality. Explainable outputs—saliency on HRV trends, sudden load spikes, or stride changes—help coaches justify adjustments.
Iottive supports end-to-end pipelines from sensor ingestion to model deployment, enabling explainable outputs that teams can trust across multiple sports. Ongoing retraining and governance ensure models remain reliable as rosters and seasons evolve.
Key Buying Criteria: Features That Actually Prevent Injuries
Buying the right system starts with clear validation of what each sensor measures and why it matters for day-to-day training. Focus on signal fidelity and published accuracy, not only marketing claims.

Sensor stack essentials
Core sensors should include reliable heart rate and HRV, accelerometers, gyros, and optional EMG for muscle load. Pair GPS or IMU motion capture with heart streams for richer performance and prevention signals.
Real-time alerts and analytics
Edge alerts on the band reduce reaction time, while cloud analytics provide trend scoring like readiness and strain. Both are needed for immediate and longitudinal decisions.
Practical checks
- Battery life and comfort determine adoption and data completeness.
- Calibration workflows and placement guides keep metrics consistent across seasons.
- Confirm BLE throughput, pairing stability, and data portability to avoid gaps and vendor lock-in.
“Demand published validation—test-retest reliability and field accuracy under movement and sweat.”
| Criterion | Why it matters | What to verify |
|---|---|---|
| Sensor fidelity | Accurate metrics drive action | Published AUC, test-retest, placement consistency |
| Alerts (edge vs cloud) | Different decision windows | Latency specs, offline edge inference, cloud trend models |
| Comfort & battery | User adherence and coverage | Hours per charge, strap options, sweat resistance |
| Integration & validation | Scales to workflows | APIs, BLE throughput, clinical or field studies |
Top Categories and Leading Devices for Athletes and Teams
Top-tier platforms focus on what teams need most: clear load metrics and recovery scores that guide daily decisions.
Load and movement tracking: Catapult and STATSports capture external load, high-speed runs, and accelerations using GPS and IMU arrays. Their dashboards break sessions into positional heatmaps and sprint counts. Coaches use that output to quantify session intensity and manage minutes.
Recovery and readiness: WHOOP and Oura aggregate HRV, sleep stages, and strain into daily readiness scores. Polar blends heart rate and GPS into training guidance for endurance and mixed sessions. Teams use these scores to tune training dose and reduce fatigue-related injuries.
Typical workflows knit both streams together: pre-session readiness checks, in-session monitoring, and post-session debriefs with positional and physiological context. Movement signatures help coaching staff spot late-game fatigue and change substitutions to protect players.
“Centralizing data from multiple sources creates a single source of truth for coaching, science, and medical teams.”
| Category | Leading Options | Coach Value |
|---|---|---|
| External load & movement | Catapult, STATSports | High-speed metrics, session intensity |
| Recovery & readiness | WHOOP, Oura, Polar | HRV, sleep, strain to guide recovery |
| Integration & export | Iottive-enabled platforms | Unified dashboards, custom analytics |
Pricing and ecosystem: Expect hardware bundles, annual software licenses, and export options. Verify API access and compatibility with athlete management systems before buying.
Validation and fit matter: choose form factors—vests, straps, or wrist—based on sport and comfort to ensure compliance across pros, colleges, academies, and ambitious amateurs. Iottive can integrate these devices into unified mobile apps and cloud dashboards to simplify workflows across coaching, science, and medical teams.
From Data to Decisions: IoT Health Analytics Platforms
Good platforms filter noise and surface trends that matter for performance and prevention across a roster. Coaches need clear, contextual insights that link load and readiness to practical actions.
Dashboards coaches use: training load, ACWR, and trend spotting
Core widgets should show ACWR charts (highlight >1.5), readiness scores driven by HRV and sleep, and squad-level injury flag trends.
Multi-source feeds—wearable streams, EHR notes, and session logs—raise signal quality. Context matters: travel, heat, and schedule congestion change how coaches read a trend.
Integrations with EHRs, athlete management systems, and mobile apps
Role-based access keeps health data private while giving S&C, medical, and coaches tailored views. Near real-time sync lets staff make on-the-fly adjustments during practice.
Iottive provides cloud and mobile integration that pulls BLE device data, applies models, and surfaces coach-ready insights for training and recovery decisions.
- Rate and threshold alerts trigger tapered sessions or modified drills to prevent overload.
- Model monitoring and periodic re-training keep predictions aligned with roster changes.
| Widget | Core Signal | Coach Action |
|---|---|---|
| ACWR chart | Acute/chronic load (threshold >1.5) | Reduce sprint volume; modify session |
| Readiness score | HRV decline + poor sleep | Assign recovery modalities; limit minutes |
| Trend board | Squad & position flags | Compare roles; prioritize rehab |
| Integration log | EHR & session notes | Document context for return-to-play |
“Analytics platforms turn raw streams into timely decisions that preserve performance and reduce risk.”
Sport-Specific Guidance: Matching Devices to Your Discipline
Sport-specific monitoring focuses data collection where movement and load matter most.
Field play: Recommend GPS vests plus IMUs to capture high-speed runs, accelerations, and decelerations. This combo helps coaches spot load spikes that signal higher soft-tissue risk.
Court play: Use IMU-rich wearable devices to track jump counts, landings, and lateral loads. Those signals guide training programs that reduce overuse and protect performance.
Endurance: Runners and triathletes benefit from gait IMUs, cadence, ground contact time, and heart rate pairing. These metrics tune training programs and help prevent repetitive strain.
- Combat & contact: include impact sensors to log collision load and flag acute head or soft-tissue events.
- Universal: track sleep and HRV across all disciplines to separate under-recovery from under-fitness.
- Practical checks: follow placement rules, confirm competition compliance, and verify in-game tracking allowances.
How to adjust training: Use readiness and load dashboards to progress volumes gradually and avoid ACWR spikes. Clear coaching cues from platform analytics make decisions faster and keep data continuous as teams scale.
“Choose platforms that translate sport-specific movement patterns into clear coaching actions and scale from an individual to a full roster without breaking data continuity.”
Security, Privacy, and Compliance for Athlete Data
Trust depends on mixing robust encryption with simple, revocable consent for each participant.
Protecting sensitive health and performance data starts with proven technical controls and clear policies. Iottive implements secure data storage with AES-256 at rest and TLS 1.2+ in transit to protect device‑to‑app and app‑to‑cloud pathways.
Encryption, access control, and consent practices
Use role-based access so coaches view training metrics while medical staff manage protected health records. Keep audit logs for every access and change to support accountability and compliance readiness.
Standardize digital consent and revocation flows. Tell athletes what data is collected, why it is used, who can see it, and how long it is kept.
- Encrypt in transit (TLS 1.2+) and at rest (AES-256).
- Limit collection with privacy-by-design and defined retention windows.
- Run bias checks on algorithms and explain model outputs to avoid opaque decisions.
- Deliver signed firmware updates to prevent tampering at the device level.
Policy alignment matters: follow HIPAA-adjacent practices where relevant and adapt to league or institutional rules. Clear communication preserves trust and lowers legal and ethical risk.
“Transparent consent, strict controls, and explainable models keep monitoring useful while protecting athlete rights.”
Iottive pairs secure architecture with consent workflows to help organizations meet regulatory needs and foster adoption across the industry.
Implementation Playbook: Pairing, Syncing, and Scaling
A smooth implementation depends on enrollment workflows, firmware hygiene, and practical coaching buy-in.
Build reliable BLE apps and update paths first. Develop custom BLE pairing flows that support QR-code enrollment and automated profile assignment. Use Nordic DFU libraries or equivalent to manage secure firmware updates and schedule DFU windows during low-activity times.
Design mobile-cloud sync rules that permit offline capture and catch-up uploads. This prevents data loss during travel or weak connectivity. Define naming conventions so each athlete maps to the right roster and position across seasons.
Pilot to rollout: onboarding and training
Start with a motivated subgroup to validate placement, calibration, and alert thresholds. Iterate quickly and document calibration steps.
Train coaches and staff in interpreting readiness, load, and alert types. Provide concise SOPs for game days versus training days and include backup devices and sync contingencies.
- Plan provisioning and scaled pairing with QR enrollment and automated profile assignment.
- Use DFU workflows for non-disruptive firmware updates during off-hours.
- Set mobile-cloud rules for offline capture and catch-up uploads to avoid gaps.
- Pilot placement and calibration, then expand after validation.
- Deliver coach and athlete education on care, charging, and interpreting data.
Operationalize QA and measure outcomes. Implement missing-data flags, outlier detection, and dashboards for sensor health. Track availability, performance markers, and incident rates to document ROI and guide continuous improvement.
“Plan provisioning, secure updates, and staff training before full roster rollout to keep monitoring consistent and reliable.”
| Phase | Core Actions | Success Metric |
|---|---|---|
| Pilot | Enrollment, placement checks, threshold tuning | Data completeness >95%, calibrated alerts |
| Scale | Mass pairing, DFU scheduling, roster mapping | Zero pairing backlog; stable sync across sessions |
| Operate | QA dashboards, SOPs, staff refresh training | Reduced downtime; measurable availability gains |
How Iottive Helps: End-to-End IoT/AIoT Solutions for Wearable Injury Prevention
Iottive packages BLE pairing, secure sync, and coach-ready dashboards into a single rollout plan that cuts time-to-value. The company builds custom BLE mobile apps, integrates multiple sensor stacks, and deploys secure cloud analytics to turn raw data into clear performance and prevention insights.
Custom BLE apps, analytics, and smart device integration
Fast pairing and stable streaming matter. Iottive delivers mobile apps that pair reliably, handle DFU updates, and present unified dashboards across Catapult, STATSports, WHOOP, Oura, and Polar.
Edge alerts and cloud pipelines combine immediate notifications with deeper trend models so coaching staff can act during training and review long-term data for load management.
Industries served: cross‑industry rigor meets sports-ready know-how
Iottive applies lessons from Healthcare, Automotive, Smart Home, Consumer Electronics, and Industrial sectors to sports programs. That cross-industry rigor boosts security, calibration, and deployment speed.
Build your custom platform: cloud, mobile, and analytics pipelines
- Custom BLE apps that pair quickly and stream reliable data.
- Integration of multiple devices and sensors into one platform for unified insights.
- Secure cloud architectures with analytics pipelines and role-based access.
Get started: scope a pilot or full rollout at www.iottive.com or contact sales@iottive.com for a roadmap tailored to training, heart rate streams, and roster scale.
Conclusion
A clear decision rule that ties a metric to an immediate action is the difference between noise and prevention.
Invest in validated systems that convert continuous data into simple coach-facing actions to prevent injuries and sustain performance.
Readiness frameworks that blend heart rate variability, sleep, and load guide daily training and support faster recovery. Proven thresholds—HRV drops >20% and ACWR >1.5—help teams act before problems grow. Elite studies report AUCs up to ~0.87 for risk models, showing real value when models are explainable and governed.
Start with a pilot, formalize decision rules, protect privacy with encryption and consent, and scale with unified dashboards that serve coaches and athletes. Iottive stands ready to build the custom BLE apps, integrations, and analytics you need to operationalize prevention and elevate athlete performance.Contact www.iottive.com | sales@iottive.com.
FAQ
What does a predictive training monitor do for performance and safety?
A predictive training monitor collects physiological and movement data to flag rising risk markers such as fatigue, abnormal gait, or elevated load. It helps coaches and staff adjust sessions, prescribe recovery, and reduce the chance of time-loss problems by turning raw metrics into actionable guidance.
Which sensors matter most for early risk detection?
Core sensors include optical or chest heart-rate measurement, heart-rate variability (HRV), accelerometers and gyroscopes for movement, and electromyography for muscle activity. These feed analytics that detect overload, asymmetry, and neuromuscular fatigue.
How does real-time monitoring change training decisions?
Real-time alerts let staff modify intensity or volume immediately—swap a drill, shorten a set, or initiate recovery protocols. That reduces cumulative stress and lowers the chance of sudden breakdowns linked to fatigue and poor movement patterns.
What role do edge and cloud models play in risk scoring?
Edge models deliver instant scoring and alerts on the unit for immediate action. Cloud models handle heavy analytics, trend detection, and cross-athlete comparisons. Combining both provides fast responses and deep longitudinal insight.
Can these systems work across multiple sports and levels?
Yes. Transferable models and sport-specific calibration allow platforms to adapt to team football, track and field, or individual endurance disciplines. Validation studies and localized training data improve accuracy for each use case.
How should teams validate device accuracy and claims?
Look for independent validation papers, peer-reviewed studies, or third-party lab tests. Check raw-signal access, calibration procedures, and whether the vendor shares algorithms, error rates, and population details used in testing.
Which commercial options focus on load and movement tracking?
Proven systems include Catapult and STATSports for external load and positional analytics. These platforms emphasize GPS, inertial sensing, and team-level dashboards used by professional programs.
What about devices geared to recovery and readiness?
Products such as WHOOP, Oura, and Polar provide sleep, HRV, and readiness insights. They prioritize overnight monitoring and recovery scoring to guide day-to-day readiness decisions for training and competition.
How do analytics platforms translate data into coach-facing dashboards?
Platforms compute training-load metrics like acute:chronic workload ratio (ACWR), session RPE aggregates, and trend lines. Dashboards highlight outliers, flag rising risk, and enable drill-downs into individual sessions and wearable metrics.
Can platforms integrate with athlete medical records and management systems?
Most enterprise platforms support integrations via APIs or HL7/FHIR connectors to link with electronic health records and athlete management systems. This creates a consolidated view for clinicians and performance staff.
What security and privacy measures should teams require?
Require end-to-end encryption, role-based access control, anonymization for research, and clear consent workflows. Confirm compliance with applicable laws and industry standards to protect personal health information.
How do organizations run a pilot before full rollout?
Start with a small cohort, test pairing and firmware update flows, validate data quality, and iterate dashboards. Use pilot feedback to refine protocols, training for staff, and integration points before scaling.
What are practical battery-life and comfort expectations?
Aim for multi-day battery life with quick charging for team use. Comfort depends on form factor—wristbands suit recovery monitoring, while chest straps or garment sensors often yield higher signal fidelity during intense activity.
How important is signal calibration and ongoing quality control?
Vital. Regular calibration, signal verification, and artifact filtering ensure reliable metrics. Poor data quality leads to false alerts or missed issues, undermining trust in the system.
How does federated learning or explainable modeling help deployment?
Federated approaches let organizations improve models without sharing raw data, protecting privacy. Explainable models provide interpretable reasons for alerts, helping coaches accept recommendations and adjust training with confidence.
What industry experience should a solution partner offer?
Seek vendors with cross-domain expertise—healthcare data handling, embedded BLE app development, cloud analytics, and experience deploying for teams or clinics. That mix shortens time to value and eases regulatory navigation.
Which metrics should appear on a minimal viable dashboard?
Include heart-rate trends, HRV baseline, load per session, movement asymmetries, sleep quality, and a composite readiness or recovery score. These provide an actionable snapshot without overwhelming staff.
How can smaller programs access high-quality monitoring affordably?
Prioritize essential sensors and cloud subscription tiers that scale. Use phased deployments, open APIs to combine lower-cost devices with centralized analytics, and leverage shared pilot data to negotiate better pricing.
What legal and ethical issues arise when monitoring minors?
Obtain parental consent, limit data sharing, anonymize datasets for research, and enforce strict access controls. Comply with child-protection laws and the policies of governing bodies to avoid liability.
How do sleep and recovery tracking factor into reducing workload-related harm?
Sleep metrics and recovery scores reveal insufficient rest or autonomic strain that raise vulnerability to overuse problems. Incorporating these measures lets staff adjust load and prescribe targeted recovery interventions.
What makes a roster-wide implementation successful?
Clear protocols, staff training, athlete buy-in, reliable pairing workflows, and routine data reviews. Success hinges on turning alerts into simple, consistent actions that integrate with daily routines.
How should teams measure return on investment?
Track reductions in time-loss incidents, days missed, rehospitalization or re-injury rates, and performance continuity. Also measure staff time saved through automation and improvements in player availability.