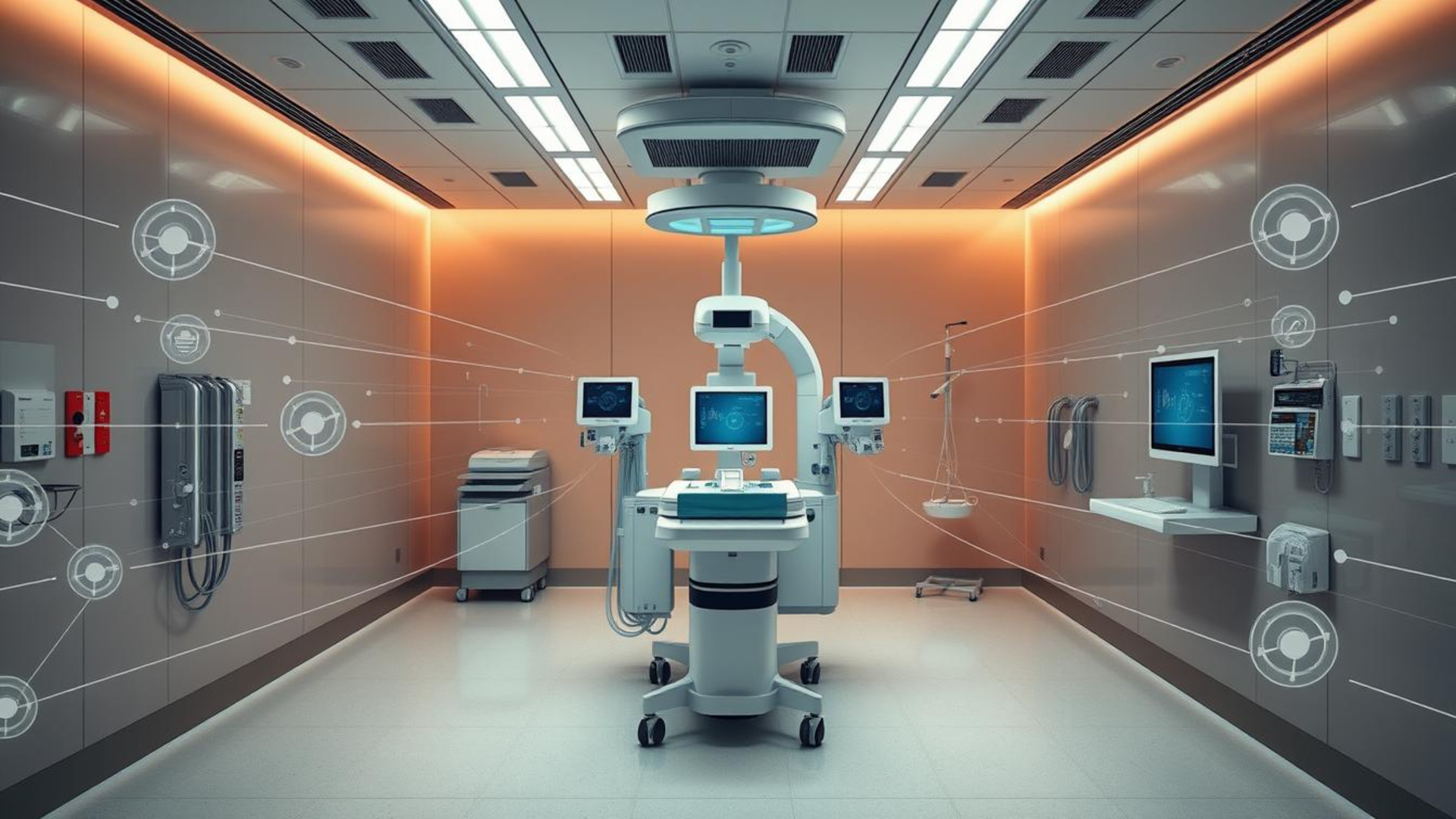
It started with a single delay: a respiratory cart misplaced during a midnight emergency sent a team hunting through corridors while a patient waited. That small delay showed how much depends on clear visibility of medical equipment and fast response.
Today, real-time tracking and connected systems cut search time and keep devices ready for care. Tagging, BLE beacons, and gateways feed centralized platforms with data on location, condition, and usage.
Hospitals and healthcare leaders now prioritize tracking and monitoring to reduce losses, lower wait time, and improve management of medical equipment. Analytics help predict maintenance, flag unauthorized movement, and boost uptime.
Iottive delivers end-to-end solutions—BLE app development, cloud integration, and tailored platforms—to help hospitals scale deployments and align technology with workflow goals. This article will cover core technologies, intelligence layers, use cases, outcomes, challenges, and a rollout roadmap.
Key Takeaways
- Real-time data and tracking reduce delays and speed access to equipment.
- Integrated tags, sensors, and cloud systems enable better utilization and maintenance.
- Analytics cut losses and support compliance while extending device life.
- BLE, RFID, gateways, and mobile apps work together in scalable solutions.
- Iottive offers consultative, end-to-end services to align technology and process.
Why hospitals need smart asset monitoring now
Healthcare leaders now see clear market signals that device connectivity will reshape patient care workflows. Rapid double‑digit growth for connected systems and intelligent edge solutions is driving adoption across the U.S.
![]()
Market signals: fast growth and wide adoption
The IoT market in healthcare is set to grow from USD 53.64B (2024) to USD 368.06B (2034) at a 21.24% CAGR. The AIoT segment is projected to expand even faster. Over 60% of hospitals already deploy connected devices, and 75% of executives expect meaningful outcome gains.
Operational pressures: staff, wait times, and rising costs
Staff shortages and high demand lengthen queues and strain clinicians. Equipment search time delays treatment and adds to patient wait times.
| Challenge | Impact | How tracking helps |
|---|---|---|
| Equipment scavenging | Delayed procedures, longer wait times | Real‑time location reduces search time |
| Underused purchases | Higher capital and replacement costs | Utilization data reduces duplicate buys |
| Scale & governance | Data silos, compliance risk | Cloud integration and policies enable secure scale |
Connected data speeds decisions at the point of care. That leads to faster treatment, better patient monitoring readiness, and an average 26% operations cost reduction. Iottive helps align BLE app development, cloud integration, and device solutions to clinical workflows. Contact: www.iottive.com | sales@iottive.com.
smart hospital asset monitoring, smart IoT Assets monitoring using, AIoT
When devices report location and condition, teams move from searching to acting.
Integrated monitoring connects tags, beacons, RFID, and Wi‑Fi to a central platform. That platform streams location, condition, and usage so staff and clinicians see equipment status in real time.

How this works: tracking gives precise location; monitoring adds condition and use data for maintenance and alerts. Hospitals build taxonomies to map items to service lines, care pathways, and departments for clearer reports.
- Standardize tags and data models for consistent reporting.
- Unify dashboards so clinical teams, biomed, and supply chain share one source of truth.
- Use analytics to cut duplicate requests, rentals, and downtime.
| Capability | Value | Outcome |
|---|---|---|
| Location tracking | Quick finds, reduced search time | Faster treatment starts |
| Condition & usage monitoring | Predictive maintenance, lifecycle data | Lower failures, longer equipment life |
| On‑device intelligence | Edge alerts and filtered events | Timely interventions, fewer false alarms |
Iottive designs end-to-end solutions—BLE app development, analytics, and cloud/mobile integration—to orchestrate sensors, apps, and platforms into one cohesive monitoring system. Contact: www.iottive.com | sales@iottive.com.
The core technologies behind real-time hospital equipment tracking
Reliable location services begin with layered architecture: tags and badges at the edge, a location engine to interpret signals, and centralized management to present status to staff and clinicians.
RTLS foundations combine tags/badges, network backhaul, and geospatial software to deliver facility-wide visibility. Systems stream real-time data into dashboards and hospital systems like EHR, CMMS, and BMS so teams see device status and maintenance priorities instantly.

Choosing the right mix
- BLE beacons fit wide coverage and low power with room-level accuracy.
- RFID offers low cost per tag for inventory and check-in workflows.
- Wi‑Fi leverages existing networks for building-wide tracking with moderate precision.
| Technology | Strength | Best use |
|---|---|---|
| BLE beacons | Low power, scalable | Wide-area tracking, long battery life |
| RFID | Low cost, quick reads | Asset counts, supply areas |
| Infrared/Ultrasound | Room-level precision | ICU, OR, secure rooms |
| Sensors (motion, temp) | Condition & utilization | Cold chain, usage analytics |
Staff search time averages 72 minutes per shift and 10–20% of mobile assets go missing during life, often costing thousands each. Robust governance for device identity and firmware keeps deployments secure and manageable. Iottive integrates BLE, RFID, Wi‑Fi, lighting-based RTLS, and environmental sensors into unified platforms for scalable, low-power solutions. Contact: www.iottive.com | sales@iottive.com.
From data to action: how AIoT upgrades asset tracking into intelligent operations
Connecting edge processors with clinical workflows turns raw signals into fast, useful actions at the bedside.

Edge analytics and predictive maintenance to minimize downtime
Edge analytics run on gateways and BLE-connected devices to analyze signals in seconds. This reduces time to insight and lets teams act before failures occur.
Predictive models combine usage cycles, vibration, and status to schedule maintenance windows. That lowers unplanned repairs and keeps equipment available for patient care.
Utilization analytics to curb underuse and unnecessary purchases
Usage dashboards flag idle assets and duplication across departments. Hospitals use those insights to redeploy devices and avoid needless procurement.
Real-time data on device hours and location helps healthcare providers make buying decisions that improve operational efficiency and outcomes.
Automated alerts, geofencing, and workflow optimization
Geofencing prevents unauthorized movement and triggers alerts tied to staff tasking and ticketing systems. Automated workflows reduce manual overhead and speed response time.
In emergencies, AI-driven escalation speeds patient monitoring alerts and ensures critical equipment is routed to the right unit.
- On-device models summarize events locally and sync to cloud services for long-term analysis.
- Governance and KPI feedback loops refine models to improve uptime and care readiness.
Iottive delivers end-to-end solutions that combine edge intelligence, cloud ML, and mobile workflows to turn tracking data into measurable operational benefits. Contact: www.iottive.com | sales@iottive.com.
High‑impact hospital use cases that improve care and costs
Minute‑by‑minute visibility of devices turns long searches into immediate action at the point of care.
Locating critical medical equipment in seconds
Instant location cuts wait times and gets clinicians to treatment faster. Staff searching averages 72 minutes per shift; reducing that time frees clinicians for patient care. Iottive deploys BLE RTLS and mobile apps so teams find pumps, monitors, and carts in seconds.
![]()
Safeguarding mobile assets and preventing theft or loss
Between 10–20% of mobile assets are lost or stolen, with average loss near $3,000 per item. Geofencing, alarms, and chain‑of‑custody logs cut losses up to 35% and keep high‑value equipment visible across departments.
Enhancing staff and patient safety
RTLS badges with discreet panic buttons speed response and improve staff safety. Location tags also record status and movement to support audits and compliance.
Wayfinding and patient flow
App‑based wayfinding guides patients to appointments and updates wait times in real time. This reduces late arrivals, eases congestion, and smooths patient throughput.
| Use case | Primary benefit | Measured impact |
|---|---|---|
| Rapid equipment location | Faster treatment starts | Less staff search time; quicker care |
| Theft & loss prevention | Protected inventory | Up to 35% fewer losses; lower replacement costs |
| RTLS badge safety | Faster incident response | Improved staff safety and compliance logs |
| Patient wayfinding | Smoother arrivals & flow | Reduced wait times; better patient experience |
Iottive ties BLE RTLS, panic‑alert badges, and mobile apps into hospital systems so healthcare providers realize measurable operational efficiency. Contact: www.iottive.com | sales@iottive.com.
Evidence that smart monitoring works: measurable outcomes and market benchmarks
Hospitals that deploy real‑time tracking report clear, quantifiable gains in operations and patient care.
Clinical studies and vendor benchmarks show major benefits. Remote patient monitoring can cut readmissions by up to 50% (45% for heart failure). Systems that surface device status and location reduce patient wait times by about 50% and lower operations costs by roughly 26%.
Reduced readmissions, shorter wait times, and lower losses
Visibility into equipment and patient data speeds treatment and improves patient outcomes. Loss prevention programs using geofencing and alerts have trimmed theft and loss up to 35%.
Proven ROI: fewer replacements, better uptime, and higher staff productivity
Fewer replacements come from better utilization and condition-based maintenance. Predictive maintenance raises uptime and reduces emergency repairs.
- Staff search time drops from an average of 72 minutes per shift, freeing clinicians for care.
- Fewer duplicate purchases lower capital costs and procurement cycles.
- Dashboards and KPIs let hospitals track ROI across departments and sustain benefits.
Iottive benchmarks success on uptime, search time reduction, loss prevention, and productivity. Their reporting tools deliver the real-time data and insights executives and clinicians need to prove operational efficiency and improved patient outcomes. Contact: www.iottive.com | sales@iottive.com.
Implementation realities: challenges and how leading hospitals overcome them
Successful rollouts start with realistic site surveys and a cross‑team plan for coverage, power, and change management.
Infrastructure and coverage
Plan for multi‑floor designs that map signal paths and interference. Concrete, ducts, and large equipment create dead zones. Use floor‑by‑floor site surveys and redundancy to maintain continuous operations.
Battery life and device management
Choose low‑power BLE tags, duty cycling, and centralized device management. Firmware scheduling and bulk provisioning cut maintenance work and extend tag life.
Security, compliance, and governance
Encrypt data in transit and at rest. Apply identity controls, role‑based permissions, and HIPAA‑aligned logging to protect patient data and ensure compliance.
Change management and pilots
Train staff with role‑based sessions and super‑user programs. Run focused pilots to validate coverage, accuracy, and workflow fit before scaling.
| Reality | Mitigation | Outcome |
|---|---|---|
| Coverage gaps | Site surveys, repeaters, multi‑antenna design | Floor‑level accuracy, fewer blind spots |
| Battery churn | Low‑power tags, duty cycles, remote updates | Lower maintenance, predictable replacement |
| Compliance risk | Encryption, access controls, audit logs | HIPAA alignment, safer data handling |
Cross‑functional teams from IT, biomedical engineering, nursing, and facilities keep projects on track. Iottive designs resilient architectures, low‑power BLE tagging, secure cloud/mobile integrations, and clinician‑centered training plans to help hospitals overcome these challenges. Contact: www.iottive.com | sales@iottive.com.
Blueprint for rollout: an end-to-end roadmap hospitals can follow today
Begin deployment by mapping every device and its status so teams work from a single, trusted inventory. This creates a reliable data foundation and reduces duplicate work during later phases.
Inventory audit and asset taxonomy to set a reliable data foundation
Start with a full inventory audit that records type, value, service years, and operational status for each piece of equipment.
Build an asset taxonomy that links items to service lines, maintenance schedules, and role-based access. This supports consistent reporting and faster decision-making.
Smart tagging with BLE/RFID and integrating with EHR/CMMS/BMS systems
Select tagging—BLE or RFID—based on coverage, accuracy, and power needs. Tags deliver real-time location and status so teams find devices faster.
Integrate tracking events with EHR, CMMS, and BMS to sync scheduling, billing, and compliance with clinical workflows.
“Run a pilot in a high-impact area to validate accuracy, workflow fit, and user experience.”
- Define KPIs, governance, and data models for unified reporting.
- Pilot in ED or ICU, then expand by floor or service line with feedback loops.
- Train staff on mobile apps, dashboards, and escalation procedures tied to device events.
Establish maintenance routines and device management policies for tags, gateways, and apps to keep uptime high and replacements predictable.
Iottive provides discovery workshops, inventory audits, BLE/RFID tagging, and integrations with EHR, CMMS, and BMS to accelerate rollout and reduce integration risks. Contact: www.iottive.com | sales@iottive.com.
Conclusion
Reliable equipment visibility turns data into faster bedside care and fewer delays.
Connected tracking and monitoring make it easier for staff to find what they need when seconds matter.
Good systems combine inventory, taxonomy, tags, and integrations so clinical teams work from one source of truth. This approach supports better patient care and operational efficiency.
Safety benefits include geofencing, panic alerts, and environmental sensors that protect patients and staff. Ongoing maintenance and governance keep devices dependable and compliant.
Start with a clear roadmap—audit inventory, define taxonomy, tag equipment, and link data to clinical systems. Measured programs deliver lower costs, better patient outcomes, and higher staff satisfaction.
Iottive is ready to partner with your hospital to design and deliver solutions that elevate patient care and operations. Contact: www.iottive.com | sales@iottive.com for a discovery call to align technology with clinical and operational goals.
FAQ
What is real-time equipment tracking and why does it matter for patient care?
Real-time equipment tracking uses wireless tags, sensors, and location engines to show where devices and supplies are at any moment. This reduces time staff spend searching, speeds treatments, and lowers costs from lost items. Faster access to ventilators, infusion pumps, or wheelchairs improves outcomes and reduces patient wait times.
Which technologies are commonly used to locate and monitor devices across a multi-floor facility?
Facilities typically combine BLE beacons, RFID, and Wi‑Fi positioning with RTLS location engines. Each method balances tradeoffs: BLE and Wi‑Fi work well for wide coverage, while RFID gives high accuracy for asset control. A hybrid approach optimizes accuracy, cost, and battery life.
How does edge analytics and predictive maintenance reduce equipment downtime?
Edge analytics processes sensor data locally to detect anomalies in vibration, temperature, or usage before failures occur. Predictive maintenance schedules service based on condition instead of time alone, cutting emergency repairs and extending useful life of devices.
Can tracking systems integrate with electronic health records and maintenance platforms?
Yes. Modern solutions offer APIs and standards-based connectors to integrate with EHRs, CMMS, and building management systems. Integration enables workflow automation—automatic work orders, asset histories, and contextual alerts tied to patient charts.
How do these systems protect patient data and meet HIPAA requirements?
Vendors use encryption, role-based access, and secure networks to protect location and clinical data. Hospitals should verify HIPAA-compliant contracts, audit logs, and regular security testing. Segmentation and tokenization further reduce exposure of sensitive information.
What return on investment can hospitals expect after deploying a tracking solution?
Typical benefits include fewer equipment replacements, lower search time for staff, improved equipment utilization, and reduced procedure delays. Many health systems report measurable ROI from lower capex, higher throughput, and improved staff productivity within 12–24 months.
How do tracking systems improve staff and patient safety?
Systems with RTLS badges enable panic alerts, duress notifications, and location-based PPE reminders. They also support contact tracing, occupancy monitoring, and rapid location of emergency responders—enhancing safety and response times.
What are the main implementation challenges and how are they addressed?
Common challenges include infrastructure coverage, device battery management, and clinician adoption. Hospitals overcome these by mapping signal coverage, selecting low-power tags, staging pilots, and providing role-based training to align workflows.
How do facilities choose the right mix of tags and sensors for different clinical areas?
Selection depends on required accuracy, environment, and cost. ICUs and surgical suites often need high-precision tags; supply rooms and transport items can use lower-cost BLE beacons or passive RFID. Conducting an inventory audit and pilot tests helps define the optimal mix.
Can these systems help manage cold chain and environmental compliance?
Yes. IoT sensors can continuously record temperature, humidity, and shock, issuing alerts for excursions and maintaining audit trails for vaccines and biologics. Automated logging simplifies regulatory compliance and reduces spoilage risk.
What role does utilization analytics play in reducing unnecessary purchases?
Utilization analytics reveals underused equipment and duplication across departments. By identifying idle assets and sharing resources, hospitals avoid unnecessary purchases and free up capital for high-impact investments.
How long does a typical rollout take from pilot to full deployment?
Timelines vary, but many hospitals complete pilots in 3–6 months and scale campus-wide within 9–18 months. Faster rollouts depend on existing IT maturity, integration complexity, and stakeholder engagement.
Are location systems hard to scale across multiple sites or campuses?
Scalable platforms use centralized management, cloud services, and standardized tagging. Planning for consistent taxonomy, network design, and device lifecycle management simplifies multi-site rollouts and ongoing operations.
What operational metrics should hospitals track to measure success?
Key metrics include equipment search time, asset utilization rate, maintenance cost per device, number of lost items, procedure start delays, and staff time saved. Monitoring these KPIs demonstrates financial and clinical impact.
How can hospitals ensure strong clinician adoption and behavior change?
Involve clinicians early, map workflows, run targeted pilots, and show quick wins that reduce daily friction. Provide hands-on training, easy-to-use interfaces, and feedback loops so staff see direct benefits in care delivery.